Biocontainment Patient Care Units: 8 critical design considerations that facilitate efficiency, safety + patient-centered care
By John Andrews | Photos: Courtesy of LEO A DALY
Doctors and nurses who treat highly-infectious diseases do so at great personal risk. These are deadly illnesses for which there is no vaccine, and whether they are transmitted via bodily fluids, in the case of Ebola, or through the air, in the case of SARS, they pose a serious threat to the men and women who provide care.
The reported cases of Ebola, and the hospital-acquired infections of medical staff treating it, has caused some to question whether the traditional hospital setting is ideally suited for the care of the world’s most dangerous diseases. Many hospital administrators are looking into the design of biocontainment patient care units, special facilities that apply the techniques of laboratory biocontainment to the clinical environment. These meticulously planned and engineered facilities provide safety and peace of mind to caregivers, while facilitating staff efficiency and patient-centered care.
There are four BPCUs in the United States: a three-room unit at the National Institutes of Health in Bethesda, Maryland, a two-room unit at Emory University in Atlanta, Georgia, a five-room unit at the Nebraska Medical Center in Omaha, Nebraska and a three-room unit at Saint Patrick Hospital in Missoula, Montana. The Nebraska Biocontainment Patient Care Unit is the largest, and in many ways provides the best case study in facilities of this type. Since its activation in September 2014 for the treatment of Ebola, it has been looked to by many as the gold standard in biocontainment patient care. Although it looks like any other hospital ward, under the hood are many specialized features designed to keep staff, patients and the community safe from the diseases they treat.
The Nebraska Biocontainment Patient Care Unit, in brief
The Nebraska BPCU is designed to account for every particle of aspirated air; every scrap of clothing, waste and linen; and every inch of surface that could harbor infection.
Using specialized air handling systems, waste disposal machinery, surface materials, security systems, staff and patient throughput schemes and lab-specimen handling equipment, it is designed to offer the best possible protection against nosocomial infection.
Special design considerations are present to mitigate the mental stress felt by patients in isolation. And because of its size — five patient rooms — it offers more flexibility than other units of its kind.
Eight crucial design considerations of this unit are:
1. Isolated air handling
Renovated from an existing ward within the Nebraska Medical Center’s University Hospital, The Nebraska BPCU is sealed off from the rest of the hospital, and operates on its own dedicated air system. Incoming air is channeled via two redundant air handling units with pre-filters and HEPA filters. The HEPA-filtered exhaust air exits via redundant, high-plume dilution exhaust fans mounted on the roof.
Light fixtures, electrical outlets and light switches are sealed, in addition to entrance and patient room doors. Washable sub-ceilings are used for the protection of adjacent non-containment areas. Sheet vinyl flooring is installed with welded seams, and an antimicrobial sealant is applied to all wall and wall-to-floor seams. Exterior windows in the unit contain impact-resistant glass for protection against violent weather.
2. Negative pressure patient rooms
Patient rooms are kept at negative pressure by means of specially calibrated airflow, which prevents contaminated air from flowing into adjacent areas. Air is exchanged 15 times per hour. The air flows from “clean” to “dirty,” entering at the ceiling, and exiting at the room’s most infectious point, just above the floor at the head of the patient bed. An alarmed pressure monitor outside each door sounds if the room’s pressure falls below a certain threshold.
3. Unidirectional throughput
Staff throughput in the unit follows a clean to dirty path. The secure staff entrance leads to a clean changing room, where personal items are placed in pass-through lockers. Changing booths are provided for privacy. After passing into the vestibule, staff is prevented from returning to the changing room through the absence of a return door knob.
After completing shifts, staff exits the unit via a pass-through shower, where they “shower out” into the exit room. There, they have access to the opposite side of the same pass-through lockers used when entering.
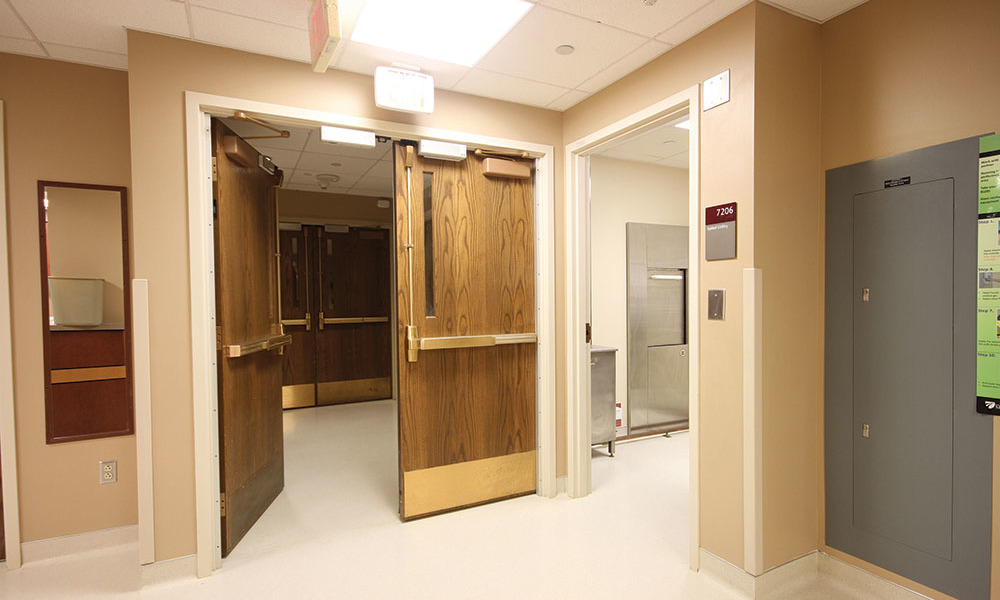
4. Secure entrance/exit
Patients and deliveries enter the unit via a secure set of air-locked double doors at the primary entrance. A second pair of doors into the vestibule will not operate until the first pair has closed. A keycard system grants access only to authorized personnel.
5. Waste handling
Soiled materials, linens and lab samples leave the unit through a separate exit outfitted with a specimen “dunk tank” and pass-through autoclave. All soiled items are placed in the autoclave, sterilized under high-pressure steam, and then put in boxes and hauled away to be incinerated. Lab specimens are disinfected in the chemical dunk tank before going to the hospital’s central lab.
6. Cleanability
The unit features washable walls and floor surfaces designed to withstand repeated cleansing with a bleach solution.
7. Flexibility
A key feature of The Nebraska BPCU is its flexibility. Five patient rooms allow the unit to function as a normal inpatient ward when not needed for biocontainment purposes. This ample size also lets the unit adapt to the varying demands of different diseases. In the treatment of Ebola, for example, unneeded patient rooms can be repurposed for other uses. These include:
a) Dirty storage: The treatment of one Ebola patient produces eight 55-gallon barrels of medical waste each day. Even with an autoclave, the purifying of this waste is a slow process, taking an average of 12 hours a day. With the autoclave limiting the rate of waste disposal, extra storage space is needed to contain the waste until it can be sent through. The unit’s flexible design allows one patient room to serve as this staging area.
b) Point-of-care laboratory: The significant loss of fluids experienced by Ebola patients requires regular lab testing. To expedite results, and avoid the extra step of purifying samples in the dunk tank, the unit’s size permits a spare patient room to be converted temporarily into a point-of-care lab.
c) Clean storage: In addition to keeping infection contained, negative-pressure rooms can also function to keep germs out. This allows a patient room to be repurposed as a clean staging area, storing medical equipment that must be kept close-at-hand in a sterile environment.
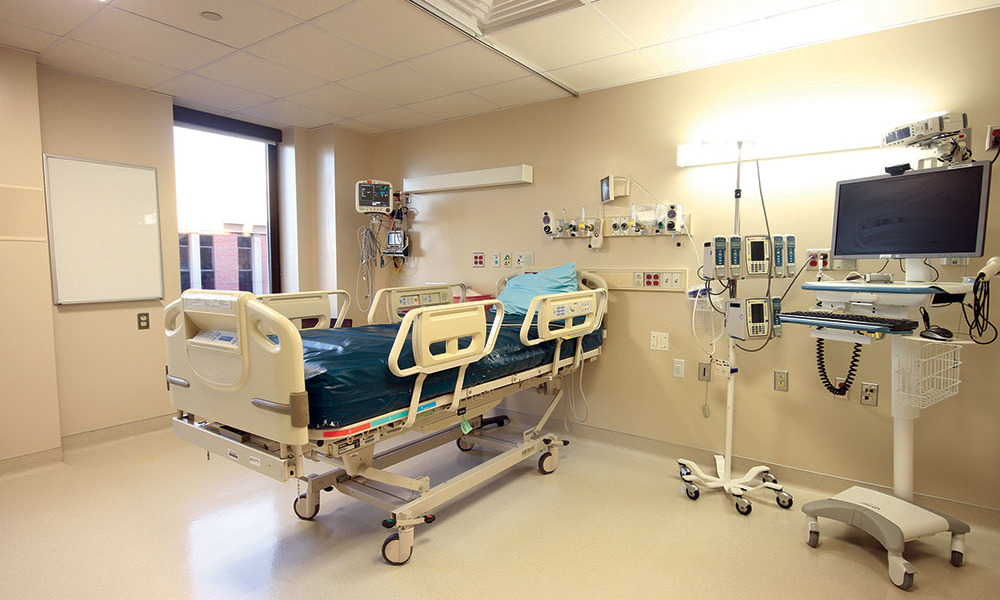
8. Patient comfort
In the sustained isolation of a BPCU, care must be taken to attend to the patient’s mental health. Large windows in each patient room provide crucial daylight and a connection to the outside world, which research suggests reduces stress and improves outcomes. The installation of video phones allows the patient to “visit” with family, and allows consulting physicians to see the patient without entering the unit.
Safe place for care
The presence of a BPCU allows the
Nebraska Medical Center to treat infectious diseases at a greatly decreased risk to caregivers. Its special air handling system allows for the treatment of airborne diseases, while its special throughput features, waste-handling equipment and flexibility enable it to treat hemorrhagic fever viruses like Ebola. By attending to the patient experience, this design also reduces the stress associated with lengthy isolation.
Author: John Andrews | Photos: Courtesy of LEO A DALY
John W. Andrews, AIA, NCARB, is vice president, senior project manager and healthcare market sector leader for LEO A DALY. He has 35 years of experience designing medical facilities, including the Nebraska Biocontainment Patient Care Unit.
Posted February 10, 2015
More Articles:
- IAPMO Publishes Manual of Recommended Construction Practices for Potable Water
- SmithGroup Promotes Andrew Brumbach to Lead Boston Health Studio
- IAPMO Hires Christoph Lohr as Vice President of Strategic Initiatives
- CDC to Address COVID-19 Impact on Legionnaires’ Disease, Present New Prevention Tools at Legionella Conference
- CxA Workshop & Exam
Apr 29, 2024 – Apr 30, 2024 - EMP Seminar & Exam at CxEnergy 2024
Apr 29, 2024 – Apr 30, 2024 - CxEnergy
Apr 29, 2024 – May 2, 2024 - PHCC West 2024
Apr 29, 2024 – May 2, 2024 - Lean in Design Forum 2024
May 1, 2024 – May 2, 2024 - IFMA’s Facility Fusion Conference & Expo
May 5, 2024 – May 7, 2024 - ASHE Academy 2024
May 6, 2024 – May 10, 2024