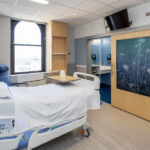
Community, culture + context key to thoughtful design
In the heart of every small town lies a vibrant community, where neighbors are like family and familiar landmarks guide the way. This is the essence of rural healthcare, as well: mutual understanding, shared history, personalized care.
The rural healthcare landscape also faces challenges that underscore the pivotal role of healthcare architecture and design in ensuring access, quality and comprehensive care.
The U.S. Department of Agriculture quantifies rural areas as those with fewer than 500 people per square mile, or fewer than 2,500 inhabitants. Rural residents live an average of 10.5 miles from the nearest hospital, compared to the suburbs’ 5.6 miles and urban areas’ 4.4 miles, according to a Pew Research Center study.
But the reality in much of the U.S. is that rural residents are much farther than that from even basic healthcare — an hour or more drive. (There are towns in Montana that are literally 300 miles from the nearest hospital for emergency care.)
Personal connection
Growing up in rural Georgia, I am deeply familiar with the healthcare challenges of residents who live in more remote locales. When I broke my arm in second grade, my father took me past one hospital to take me to the “good hospital,” which was another half hour of travel. We lost our local primary care doctor while I was in junior high, which actually hampered some of my classmates from seeing a doctor when they were ill since their parents couldn’t take off work and drive them 30-plus minutes each way.
MacGyvers in disguise
Providers and staff at rural healthcare facilities are MacGyvers in disguise. They know how to do more with less and have remarkable creativity and resourcefulness that have been passed down through the generations.
For example, one rural hospital I worked on had to find a reliable source of distilled water, but had no funding to install such a system. When my team arrived to start master planning, we discovered they were using a former moonshine still setup — with the copper tank and tubing — to get the correct water quality for their central sterile department.
The challenges in rural healthcare mirror those in urban areas, but are intensified by lower patient volumes and financial constraints. Aging infrastructure, outdated facilities and a lack of access to capital funds hinder progress. Many rural healthcare facilities were built in the Hill-Burton Era. Known formally as the Hospital Survey and Construction Act, the 75-year-old law is responsible for the construction of much of our country’s health system infrastructure.
Medicaid/Medicare, uninsured and charity patients can drain profit margins without private-pay volumes to balance the budget. And while philanthropic efforts are vital, they’re often limited by the small donor pool in these communities.
Healthcare hubs
The anxieties of rural healthcare administrators — the concerns that keep them up at night — are centered around delivering the comprehensive, quality care their communities need within the confines of these limitations.
Striving to be a community’s healthcare hub and “one-stop shop,” they struggle to maintain specialized services. For example, residents want to be able to deliver their babies close to home, but a certain number of births per year are necessary to keep an OB-GYN labor and delivery service viable.
On the other end of the spectrum, nursing homes and assisted living facilities are closing at an alarming rate, and folks are worrying that they won’t be able to age in their own towns.
Pivotal role of medical planners
Healthcare architects and medical planners have important roles to play in helping to meet the healthcare needs of residents in smaller towns and remote, less-populated areas. Understanding the distinct rural ethos is crucial.
Several years ago, I was on a team designing a replacement facility in rural northeastern Colorado within a very close-knit town of 4,000. The emergency staff would regularly have a crowd of concerned neighbors who would follow the ambulance from a person’s house to see if they were okay, whether the patient’s kids or grandkids were alone at home and needed help, etc. We ended up creating a public ER waiting room, and then a family ER waiting room beyond a secured door. This allowed the facility to accommodate community members who were truly invested in the well-being of their neighbor and their neighbor’s family.
In the past, we’ve recommended that facilities provide Wi-Fi service to the edge of their parking lot so that community members could use the Wi-Fi for multiple reasons, including mental health services.
Also keep in mind that at a rural facility, you might need larger parking spots for tractors, oversized trucks and other large vehicles. A facility we’re working with wants to provide RV parking on its replacement hospital campus so that patient families traveling from far away, as well as tourists needing medical help, can park and hook up if they need to stay a while. This also helps with parking for long-haul truckers who find themselves in need of emergency medical care while traveling on the interstate.
Whether officially designated as such, every rural hospital is a safety-net hospital. Comprehensive, high-quality care close to home in a safe, welcoming environment is essential.
How can we contribute?
- Design operational flexibility into the facility. The same staff may be covering three to four different departments.
- Initiate conversations about workflow and encourage clients to envision new ways of accomplishing the same goal — “What if we did it this way?”
- Help staff understand that design improvements aren’t only about how they work today, but about how they want to work in the future.
- Be prepared for the design process to include some tough conversations and that you might be perceived as an “outsider” stepping into their world.
- Understand that local support for projects can be vital, especially when the facility needs to ask for community help/taxes/bond initiatives to fund a major capital project. The facility and the community need to be on the same page to understand what’s needed and how much it will cost realistically.
- Ensure clients understand you are not customizing spaces for a particular staff member, but for the role.
- Be careful with HIPAA patient privacy issues. There is often an extra layer of familiarity among the rural caregiver and patient population.
- Explain the importance of meeting regulations/code, such as those required by the Americans with Disabilities Act or for redundant HVAC or electrical equipment.
- Ask more questions, perhaps using the “5 whys” (a brainstorming method in which “Why” is asked repeatedly until the root cause of a problem is identified) to challenge them. This is a good way to get at what they really need instead of what they think they need based on existing conditions.
The challenges of rural healthcare are formidable, but the potential for transformative change is equally as significant. The key is to be thoughtful in your design, considering community, culture and context.
By embracing the rural healthcare team’s creativity, empathy and talent for innovation, and applying state-of-the-art medical planning and efficient design, we can collaboratively take steps toward ensuring that quality healthcare is accessible in every corner of our diverse country.
Supporting these rural communities and their residents’ health needs is not just a local endeavor, but a national investment in well-being.