 Swedish Medical Center, Cherry Hill Campus, Seattle, Washington. ©2016 Chris Eden Photography.
Swedish Medical Center, Cherry Hill Campus, Seattle, Washington. ©2016 Chris Eden Photography. Subscribe Now
Improving Processes
By Rudy Santacroce
Lean process improvement designs enhance ICU’s techniques
Thinking of intensive care units usually brings about thoughts of worry for a serious situation. When faced with being in an ICU, either as a patient or visitor, you have to trust that the staff is performing in the best, most efficient way possible. The best utilization of the staff’s time is critical in an ICU department.
With health systems’ complex facilities and technologies, there are often opportunities to improve operational efficiency and eliminate waste in the ways staff operates within a healthcare facility. Opportunities for improvement, or the elimination of wasteful operations, can oftentimes be unrecognizable until a team of experts are brought into the situation.
CallisonRTKL’s Operational Excellence team partnered with Providence Health & Services to provide Lean design services during the pre-design of their Swedish Medical Center, Cherry Hill Campus’ Neuro ICU expansion and renovation project in Seattle, Washington.
Improving operations
The Operational Excellence team encompasses five different service lines, including process improvement, predictive analysis, value-added assessment, data analytics and change management. The team performs critical steps in order to heighten operational efficiency and eliminate waste in operations, streamline practice pattern and align staffing and technology with demand – all improving the way healthcare facilities operate.
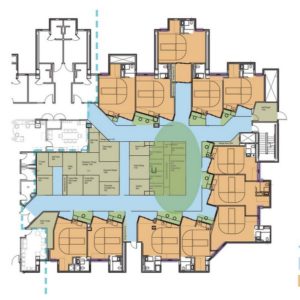 Process improvement through Lean design
Process improvement through Lean design
Even the most efficient healthcare systems consist of hundreds of complex, inter-related processes that drive waste and unnecessary expenses. Managing and analyzing these processes, through process improvement, boost operational efficiency, clinician engagement and, over time, the quality of care.
In the process improvement stage, the team engages front-line staff and key stakeholders to find and fix problems in order to ease change implementation and boost sustainability. Operations and care delivery are also assessed in major departments and services to achieve performance goals. As part of process improvement, the Lean design process, which is a collaborative approach that drives sustainable improvement, reduces waste in healthcare facilities. It is beneficial to apply Lean methodologies in the beginning of a project to better define the process by eliminating waste and variation.

CallisonRTKL’s Operational Excellence team provided Lean design services during the pre-design of the Swedish Medical Center, Cherry Hill Campus’ Neuro ICU expansion and renovation project. ©2016 Chris Eden Photography.
Examples of waste in healthcare systems include the redundant capture of information, excess supplies stored in multiple locations, wasted time looking for charts and records, patient waiting rooms and an unnecessary amount of time spent traveling through the facility.
In the Cherry Hill Campus’ Neuro ICU expansion and renovation project, before any design took place, the project team met with the client’s design user group, consisting of the peri-operative director, nursing director, nurse manager, OR manager, neuro coordinator, med/surg nurses and ancillary services representatives, to perform visioning sessions. They expressed much angst in their current environment for not only patient care functions, but logistics, transportation, EVS, food services and other disjointed functions. Floorplans were examined, and all workflow processes, metrics, key spaces impacted and total workflow distances per day were documented to begin assessing ways for improvement.
More efficiency for the Cherry Hill Campus’ Neuro ICU
“As healthcare planners and designers, we historically propose design solutions based on our intuition, beliefs or design sensibilities,” said John Jex, CallisonRTKL vice president and project manager of the architecture design team for the project. “When working with the Operational Excellence team, they brought tools to the planning and design process that analytically illustrate the difference, or benefits, between alternatives under consideration. This is Evidence-Based design at its best.”
The team provided a presentation on Lean with a special emphasis on seven opportunities for improvement where waste was occurring. The seven opportunities included:
- Waiting and the idle time for employees and equipment
- Transportation and movement not being value-added
- Processing and more work being done than necessary
- Wasted walking and movement
- Poor quality including errors and rework
- Storing excess inventory
- Overproduction at a higher quality and faster time than required
These seven areas for improvement were revisited throughout the design and process discussions, in order to reduce or eliminate waste when possible.
The goal for this project was to keep staff transportation in and around the unit to a minimum, in order to maximize the caregiver’s time with the patient, ensuring the best possible care.
By performing process improvement and Lean design methodologies, new designs led to significant improvements in workflow trip distances. A few trip distances that the team found to be in absolute need for change were the trip distances to and from the admit process, equipment storage and the trash and red bag supply rooms. The workflow distance of the admit process, including rooms for nurse monitors, Pyxis stations, storage, etc., was being traveled six times a day with a total distance of 16,890 feet per day.
The redesign decreased this distance down to 2,815 feet per day, saving staff the extra distance of 14,075 feet per day just for the admit process. Equipment storage room trip distances were decreased by 52 percent, and the trip distance to and from the trash and red bag supply room was decreased by 55 percent. Other significant improvements to workflow also took place.
Without the application of Lean methodologies and process improvement process, an excess amount of travel done by staff members would have been wasted each day. This redesign saved the staff time and maximized their interaction with patients, ultimately providing better care for the Cherry Hill Campus’ Neuro ICU patients.
Author: Rudy Santacroce
Rudy Santacroce, P.E., CSSBB, PMP, DSHS, is a vice president at CallisonRTKL. He leads the firm’s Health + Science Practice Group’s Operational Excellence Team.
Tags: Architecture, Facilities Management, Lean, Process improvement
Posted May 11, 2016
More Articles:
- CxA Workshop & Exam
Apr 29, 2024 – Apr 30, 2024 - EMP Seminar & Exam at CxEnergy 2024
Apr 29, 2024 – Apr 30, 2024 - CxEnergy
Apr 29, 2024 – May 2, 2024 - PHCC West 2024
Apr 29, 2024 – May 2, 2024 - Lean in Design Forum 2024
May 1, 2024 – May 2, 2024 - IFMA’s Facility Fusion Conference & Expo
May 5, 2024 – May 7, 2024 - ASHE Academy 2024
May 6, 2024 – May 10, 2024










