By Laurie Waggener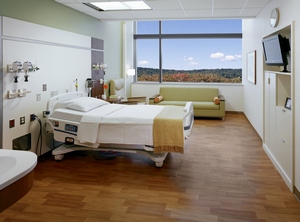
The statistics reveal that 1.7 million infections are acquired annually while admitted to a hospital:
• Most (1.3 million) were outside of ICUs
• 9.3 infections occurred per 1,000 patient-days
• One out of 22 patients will acquire an infection while hospitalized.
While research points to factors such as indoor air quality having a direct influence on infection control, consideration must be also given to the inanimate environment and spatial considerations. In other words, the walls, and especially surfaces, of objects adjacent to where the patient receives care and where the healthcare worker may inadvertently contaminate their hands and clothing.
Spatial considerations and surfaces
There is a plethora of evidence correlating a decrease in infection rates when there is a greater physical separation, isolation and space per patient in the acute-care and long-term healthcare setting. Of all the modes of transmission, providing appropriate space per patient is correlated with success rates in the prevention of transmission of infectious diseases. While heeding the evidence has contributed to the adoption of the 2006 AIA guidelines requiring new construction of single occupancy acute-care patient rooms, accessing this evidence when planning other hospital departments such as ED observation units and pre–op/holding and recovery is crucial.
Research reveals the surfaces most contaminated with multi-resistant organisms are within the area immediately adjacent to a patient such as the overbed table, the cubicle curtain, the bed rail, the infusion pump, the sink, faucet handles, blood pressure cuffs and the hard copy chart. These inanimate objects have one thing in common — all are located within 3–5 feet above finished floor. This is just the right position of the population caring for the patients.
 Knowing that less than optimal reimbursements are facing healthcare organizations as the baby boomers flood the healthcare industry, does saving upfront costs on square footage — the square footage required to get the job done safely and effectively —make sense? As the patient acuity in the U.S. rises and technological advances facilitate prompt, electronically connected care, patient rooms have become minefields of contaminated objects that can be obstacles to maintaining asepsis control during direct care. How easily are hands or a lab coat contaminated when hospital rooms are increasingly cluttered with vital, but often contaminated, equipment? Will considerations regarding the reduction in square footage in order to cut down on up-front costs be disastrous for owners given the current evidence and associated costs?
Knowing that less than optimal reimbursements are facing healthcare organizations as the baby boomers flood the healthcare industry, does saving upfront costs on square footage — the square footage required to get the job done safely and effectively —make sense? As the patient acuity in the U.S. rises and technological advances facilitate prompt, electronically connected care, patient rooms have become minefields of contaminated objects that can be obstacles to maintaining asepsis control during direct care. How easily are hands or a lab coat contaminated when hospital rooms are increasingly cluttered with vital, but often contaminated, equipment? Will considerations regarding the reduction in square footage in order to cut down on up-front costs be disastrous for owners given the current evidence and associated costs?
Evidence supports that single occupancy rooms are superior to multi-occupancy in the prevention of cross transmission. Private spaces facilitate the necessary ventilation and separation of patients with aerial transmitted infections such as influenza, TB, measles and chicken pox. Moreover, private patient rooms facilitate the new cleaning methods required to eradicate certain drug resistant organisms. If we continue to plan EDs with open bays and observation cubicles how can we facilitate the most effective cleaning method on the market, the use hydrogen peroxide vapor? Are plans that place patients in close proximity, with only a contaminated surface (privacy curtain) for separation, acceptable? It is never too soon to discuss infection-control protocols and the spatial requirements necessary to implement a successful program. It is time worth spending to discuss cleaning techniques necessary to eradicate drug resistant organisms in the inanimate environment and specify appropriate finishes and fabrics to facilitate the techniques.
Making crucial decisions through crucial conversations
In summary, crucial conversations for safety and quality healthcare delivery begin in pre-design and programming. While saving up-front costs associated with fewer square feet can be attractive, it can be costly post-occupancy considering potentially decreased reimbursements and extended lengths of stay.
Architects and owners must consider the required equipment vital for effective direct-care delivery and discuss spatial needs that facilitate care with minimal contamination of the caregiver before, during and after a procedure.
Most importantly, designers and owners need to spend time on the selection of materials and surfaces that fall within the 3-5 foot area above the finished floor. This is where the evidence exists regarding success and failures in cross transmission associated with direct contact. Until proper clinical trials are available to address the effectiveness of anti-microbial additives to items within this high-contact area, it might be wise to focus selection criteria on cleaning methods and meeting facility infection-control protocols.
Laurie Waggener, RRT, IIDA, AAHID, EDAC, is research and Evidence-Based Design leader at WHR Architects, Inc.
Editor’s Note: Read more about infection-control methods in the upcoming January/February issue of Medical Construction & Design.




