Subscribe Now
Navigate Growth and Change with Effective Space Programming
By Thomas Gunn
The way medical facilities operate must change exponentially as new technologies develop and new legislation is introduced. Effective space programming is key for optimal decision making while continually navigating growth and change.

Fundamentally, programmers and planners want to help healthcare leaders visualize a new image of how they can deliver care.
Space programming for growth requires a keen eye for facility assessment, accurate facility information and the population it serves, and the acumen that only years of experience can bring. Careful assessments help programmers and planners understand the space and its complexities to determine probable adaptive reuse or to build new facilities once they know what services are being contemplated. And, understanding adjacencies and flow are key to overcoming the inefficiencies that often exist in older buildings, or determining when it makes more sense to build new.
Effective space programming can show the best possible options for changing, expanding and improving operations. Here are insights into optimizing effective space programming:
Know where you are going
To create a balance between what is, and what is possible, the first step is to create a realistic five-year forecast that considers what will be effective. With a realistic assessment of market share, map the future plans in the context of general healthcare trends. Getting accurate numbers on today’s performance and whether that is trending up or down is important; patient satisfaction surveys are a good way to assess strengths and areas for improvement from the firsthand perspective of patients, providers and users.
The groundwork for creating the plan can result in a large amount of data, so it is important to prioritize the information and not get lost in metrics and analytics. Boiling the numbers down to the fundamental priority areas for improvement allows programmers and planners to share a concise presentation – simple charts are fundamentally important – with leadership. The key to effective communication in a space program is to break down the data so that managers can see positive and negative effects on operations and interrelationships.
Know what you have
Leaders often are not fully aware of their capacity and performance level in the context of what is happening in the industry, especially regarding new methods and technologies such as telemedicine and interventional radiology, for example. Doctors who have admitting privileges to multiple hospitals will give preference to institutions with the most state-of-the-art equipment. Leaders who are knowledgeable about changes in healthcare, and what the industry is doing to address those changes, can stay ahead and advance the care they provide so that it is the most optimal service available to patients.
All aspects of today’s processes must be considered when evaluating growth. Wait times need to be reduced using Lean process techniques to plan – step by step – how long it takes to do what needs to be done, as well as finding the optimal layout to effectively use a facility, which is key to cutting turnaround times. Well-trained staff on advanced technology will optimize a process-based layout, and investing in the best tools will ensure a hospital remains competitive in the marketplace. All these contribute to the positive outcomes that keep physicians and patients coming back.
Patients respond to a system that makes healthcare easy to understand, access and utilize, for them and their families. Healthcare can be stressful for families, so making it as simple and accessible as possible ensures greater patient satisfaction, with services like those found in an upscale hospitality environment, as well as practical amenities including Wi-Fi. Things like electronic admissions that patients can complete in advance to expedite their hospital stay give them less to think about once they arrive. Everyone’s time is valuable and the less time patients spend waiting or providing repetitive information, the happier they tend to be.
Fundamentally, programmers and planners want to help healthcare leaders visualize a new image of how they can deliver care. Technology has significantly changed the way healthcare is delivered and the key to harnessing that technology is to be responsive 24/7 and anticipate what future generations of patients will want – and delivering it quickly and effectively. These are complex concepts, but one way to simplify these complexities is to break them into fundamental interrelationships that everyone can understand, then quantify all processes and elements —such as time in terms of Lean process, cost of delivery, cost of care and tools to deliver that level and quality of care—to find opportunities for improvement. Once the basics are in place, it is easier to effectively program and plan – flexibility of space and technology – for increased volumes or change how the clinical activity is done to optimize the process and outcomes.
Measure plans in context of the present, practice flexibility
Quantifiable data collected while assessing and analyzing operations is critical when reconciling an effective plan with what is needed to get there. Fostering a relationship between a project team and healthcare leaders that is based in trust is important. The best way to do this is through total immersion of those healthcare leaders, walking them through not only the metrics and analytics but also assessments of facilities – including adaptability, adjacencies, flow and access – so they are on board with the plan and agree with where they want to go and how to get there most effectively.
Measuring the data in the context of today’s strategies and what is possible is important to plan how goals can be achieved given the existing facilities. Understanding there can be anomalies, and that metrics and analytics—however accurate—cannot predict the future, is a good reality check for healthcare leaders and project teams alike to determine direction. Focusing on realistic assumptions about the future, goals and objectives and what is possible will help to avoid frustrations and negative feedback that can happen when expectations are not met.
Be flexible. Flexibility and adaptability are the keys to responding to the changing healthcare landscape, especially in the age of rapidly changing technology and the need for instant gratification. Doctors’ offices are typically standalone facilities that lack the diagnostic and therapeutic tools needed to deliver the full range of healthcare. Today, many providers are in group practices and are moving those practices into the hospital complex so these diagnostic and therapeutic services are easily accessible, improving the delivery of care by logical integration. This works well for all hospitals integrating care modalities as a one-stop shop. Patients appreciate the convenience of getting everything done in one appointment and the hospital benefits from positive patient satisfaction outcomes.
Healthcare facilities are always changing. While decisive decision making is no small task, effective space planning can reveal the best possible options for optimizing operations while navigating growth and change.
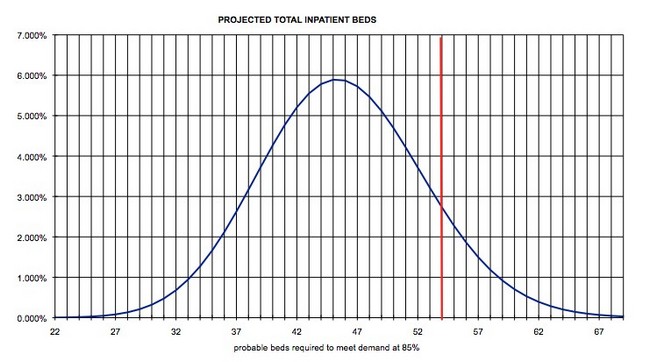
Using bell curve statistics (Poisson Mass Function Modeling), we can recommend future inpatient bed needs, based on mean bed needs, future admissions and forecast average length of stay linked to probability of demand (typically 98.5% -between one and two standard deviations). Poisson studies are generally used in context with other special modulating variance factors, such as seasonal fluctuations.
Author: Thomas Gunn
Thomas Gunn, AIA, is senior architect and senior healthcare planner with Ghafari Associates. He can be reached at 313-441-3000 or tgunn@ghafari.com.
Tags: Facilities Management, Lean, space programming
Posted April 13, 2017
More Articles:
- Tips for Scalable & Resilient Hospital Infrastructure
- Superheroes Descend on Connecticut Children’s for Groundbreaking of 8-Story Clinical Tower
- Nimon to Oversee Equipment, Technology Planning Integration at Healthcare Building Solutions
- Healthcare Facilities Among 77 Clean Air Award Recipients for 2022
- Coverings 2024
Apr 22, 2024 – Apr 25, 2024 - Hospital, Outpatient Facilities & Medical Office Buildings Summit
Apr 25, 2024 – Apr 25, 2024 - CxA Workshop & Exam
Apr 29, 2024 – Apr 30, 2024 - EMP Seminar & Exam at CxEnergy 2024
Apr 29, 2024 – Apr 30, 2024 - CxEnergy
Apr 29, 2024 – May 2, 2024 - PHCC West 2024
Apr 29, 2024 – May 2, 2024 - Lean in Design Forum 2024
May 1, 2024 – May 2, 2024










