Hospital Waste Management: Automated systems, sustainable operations and infection control
By Patrick Schultz
Hospital waste and soiled linen streams are large, complex and a source of concern for infection risk, high operational costs and inefficiency. Increasingly, hospitals consider waste management one of the most important sustainable building practices, second only to improving energy efficiency.
Improving infection control and cleanliness through sustainable operations and integrated waste management have moved to the forefront of issues facing hospitals as they seek to reduce adverse risk, improve patient safety and promote satisfaction.
Challenges, dangers associated with waste and soiled linen collection
The cycle of waste, recycling and soiled linen collection and transport in hospitals is a huge, never-ending operation. According to a 2010 survey from Practice Greenhealth, U.S. hospitals reported generating nearly 34 pounds of waste per day, per staffed bed. When factored against the number of staffed hospital beds, that’s 5.9 million tons of waste per year. Soiled linen generated per patient bed per day accounts for another 2.6 million tons per year.
At a time when hospitals are confronted with this massive task, they are also cutting annual budgets of departments considered “back-of-the-house” or “non-clinical.” This includes environmental services, or EVS, the department typically responsible for removing hospital waste and soiled linen.
Today, most hospitals have insufficient resources to move dirty material off of the patient floors and out of the facility in a timely manner. This shortfall causes a host of operational and safety challenges. Dirty material piles up in soiled rooms, hallways, at the bottom of gravity chutes and at the loading dock because EVS cannot move material to the dock quickly enough. Service elevators are used to carry dirty material down and clean material up. More troubling, staff, visitors and often patients use these same elevators continuously.
In addition to the cleanliness issues associated with the mixing of these functions, productivity and efficiency are compromised with longer elevator wait times for hospital staff. Finally, regulatory compliance may be impacted daily, resulting in life safety risks and possible fines. Hospital Consumer Assessment of Healthcare Providers and Systems scores may also be negatively impacted as limited resources are forced to focus on the collection of dirty materials instead of patient care.
Infection control issues
Beyond these operational challenges, there appears to be a potential infection control issue associated with the collection of soiled linen. A recent literature review performed by a bio-aerosol expert, concluded that “bed linens can harbor microbes, including potential pathogens” and that “microbes can be transported through the air and by touch during the routine handling and transport of soiled linen.1
Emerging infection control data taken from soiled rooms and at the bottom of chutes shows much higher exposure risk to potential airborne pathogens compared to other hospital areas. When soiled linen is agitated as it is pushed onto and off of shared service elevators, the risk rises of cross-contamination with clean supplies, dietary and a vulnerable patient population. As demand climbs for improved infection control, cleanliness, efficiency and aesthetics in hospitals, the tightening of EVS staff resources is creating an unsustainable gap between expectations and reality.
Automated waste removal systems
An attractive solution for many healthcare facilities in design or under construction is the incorporation of pneumatic waste, recycling and soiled linen collection and transport systems as part of infrastructure. These facilities are moving beyond traditional manual methods of collecting and transporting waste and soiled linen. Challenges with manual methods include the need for a large number of carts, which consumes space on patient floors, in the halls and at the dock, as well as a heavy reliance upon elevators for vertical transport. Additionally, substantial square footage is dedicated to staging rooms on patient floors and unplanned intermediate holding areas hospitalwide. All of these manual methods require substantially more labor and far greater collection and transport steps than necessary.
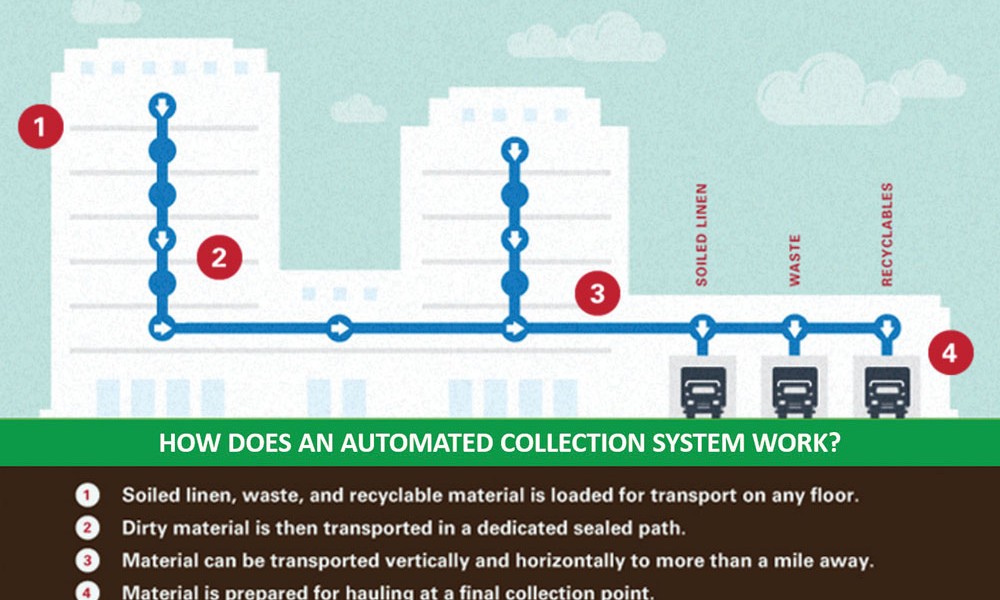
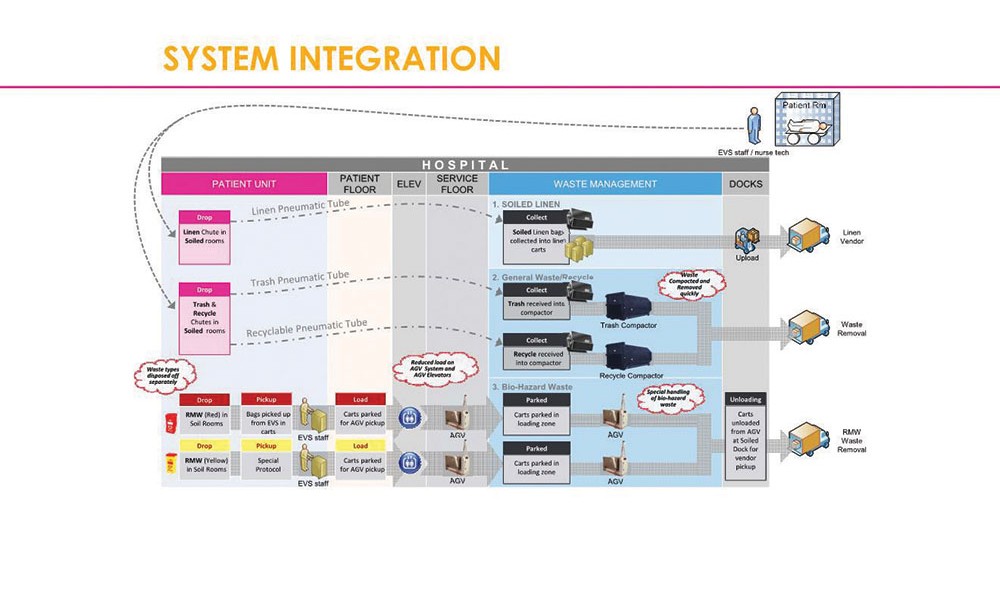
The automated solution features dedicated trash/recycling and soiled linen loading stations on patient floors and other areas of the hospital that generate waste. This simplifies and expedites the removal of waste and soiled linen from patient floors and to the dock. Once entered into a computer-controlled system, material is pulled by vacuum power at up to 60 miles per hour through a sealed, dedicated 16- or 20-inch pipe network.
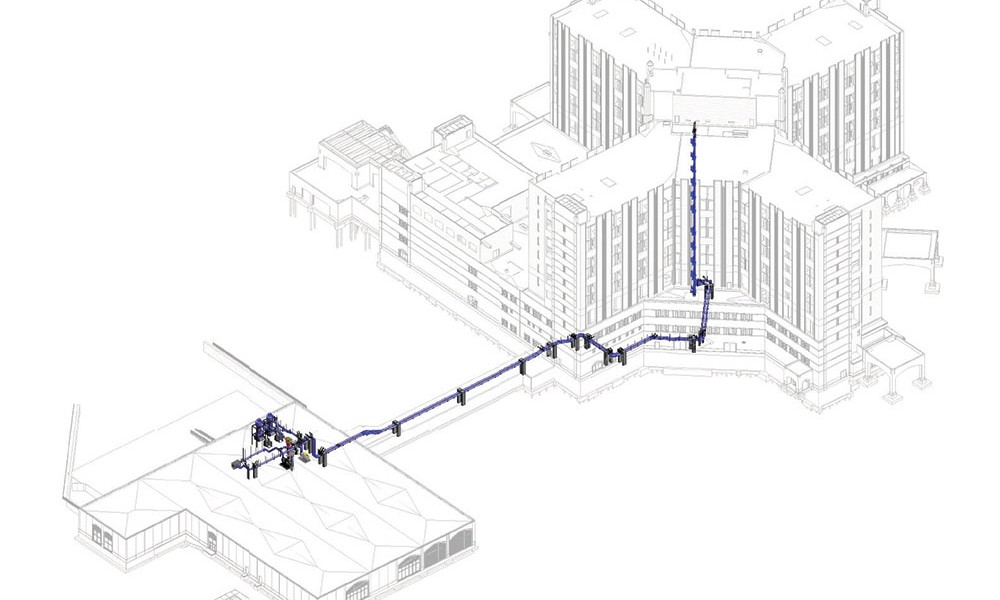
The system is installed both vertically and horizontally with material diverted automatically toward waste or recycling collectors, or to linen collectors typically located near the loading dock area. Because the system is completely sealed, human exposure time to potentially infectious materials is typically reduced by more than 80 percent compared with manual methods that rely on chutes and elevators.
Operational benefits and return on investment
Implementing an automated waste removal system will reduce the number of EVS staff required to transport, stage, unload and manage waste and soiled linen. Facility design is more efficient, as gravity chute collection rooms are eliminated and the size of soiled holding rooms is reduced. Space is freed up by not having to handle and store numerous carts at the dock and/or in halls leading up to the dock.
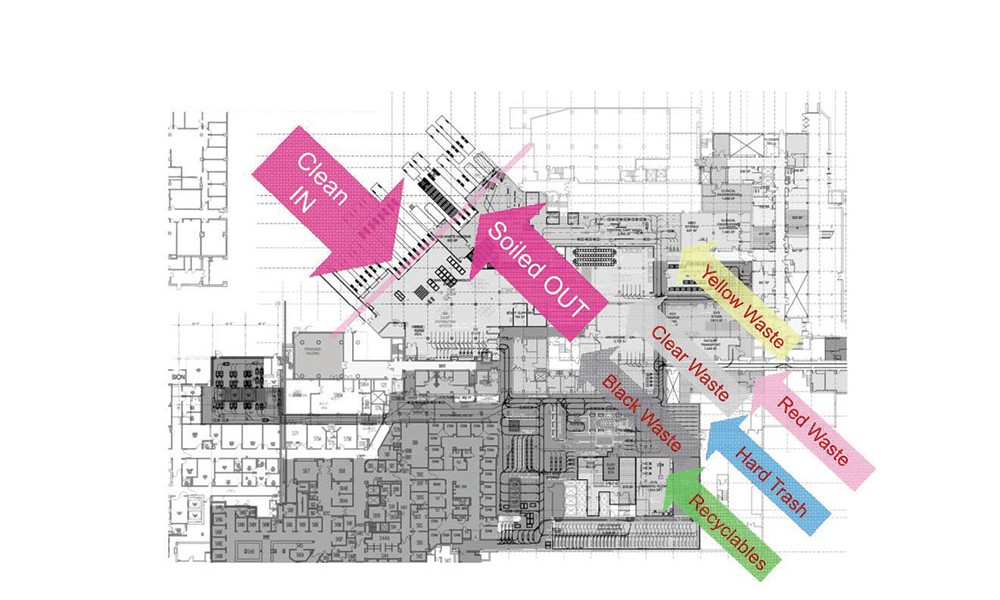
Establishing separate dirty (waste, soiled linen) and clean (food, clean linens, patients) pathways supports infection control goals by reducing the risk of direct and indirect exposure of potential pathogens. Productivity improves as EVS and housekeeping staff spend less time transporting dirty material and more time on activities that improve the patient experience. Medical staff, patients and visitors spend less time waiting for elevators. The potential cost of noncompliance with regulatory bodies is eliminated by avoiding the mixing of soiled and clean items in shared space.
Aesthetic benefits include reduced odors from soiled holding rooms, gravity chute collection rooms and loading docks. These improvements are driven by cart moves and reduced exposure on patient floors and public areas. Beyond aesthetics, hospitals are finding there’s an attractive payback with these systems, commonly in the 3-6 year range. Factors impacting the return on investment include:
- Operational cost savings
- Infection control/cleanliness
- Increased productivity
- Worker safety
- Regulatory implications
Automated systems have all the characteristics of a best practice. Not only do they improve operational efficiency, but the systems help create a less congested, healthier healing environment for patients. Automated waste removal systems provide another opportunity for hospitals to ensure sustainability, improve efficiency and reduce costs.
1 A Literature Review on the Potential for Microbial Liberation from Textiles From Residual Paths Common To Modern Healthcare Settings,” Mark Hernandez, Ph.D., P.E., Alina Handorean, Ph.D., Bharath Prithiviraj, Ph.D.
Author: Patrick Schultz
Patrick Schultz, AIA, EDAC, LEED AP, is vice president and healthcare practice leader for HKS’ Mid-Atlantic region. He has more than 25 years of experience in the planning and design of healthcare, medical research and government medical facilities nationwide. He can be reached at pschultz@hksinc.com.
Editor’s Note: Supporting research sources for this article were provided by Sarah Mueller, LEED AP, vice president, HKS Knox Advisors for Operations and Logistics. She can be reached at smueller@hksinc.com.
Posted October 2, 2014
More Articles:
- IAPMO Publishes Manual of Recommended Construction Practices for Potable Water
- SmithGroup Promotes Andrew Brumbach to Lead Boston Health Studio
- IAPMO Hires Christoph Lohr as Vice President of Strategic Initiatives
- CDC to Address COVID-19 Impact on Legionnaires’ Disease, Present New Prevention Tools at Legionella Conference
- CxA Workshop & Exam
Apr 29, 2024 – Apr 30, 2024 - EMP Seminar & Exam at CxEnergy 2024
Apr 29, 2024 – Apr 30, 2024 - CxEnergy
Apr 29, 2024 – May 2, 2024 - PHCC West 2024
Apr 29, 2024 – May 2, 2024 - Lean in Design Forum 2024
May 1, 2024 – May 2, 2024 - IFMA’s Facility Fusion Conference & Expo
May 5, 2024 – May 7, 2024 - ASHE Academy 2024
May 6, 2024 – May 10, 2024