Subscribe Now
Hybrid Operating Rooms: The Next Generation of Medical Design
 By David Magner and Angela Holcomb
By David Magner and Angela Holcomb
The medical design world is fast-paced, with new trends evolving and technologies rapidly advancing. Still yet, one innovation has stood out from the crowd lately, generating buzz from architects, hospital CEOs and caregivers alike: hybrid operating rooms.
Hybrid OR suites serve a two-in-one function, housing both diagnostic/imaging equipment and surgical equipment in one centralized location. The highly advanced suite offers the support of cardiac, vascular, oncology, neurology and other cases by allowing caregivers to verify procedures live during an operation, without ever having to move the patient or leave the room. Fewer patient transfers result in decreased procedure times, less chance of medical errors and improved patient safety and surgery outcomes.
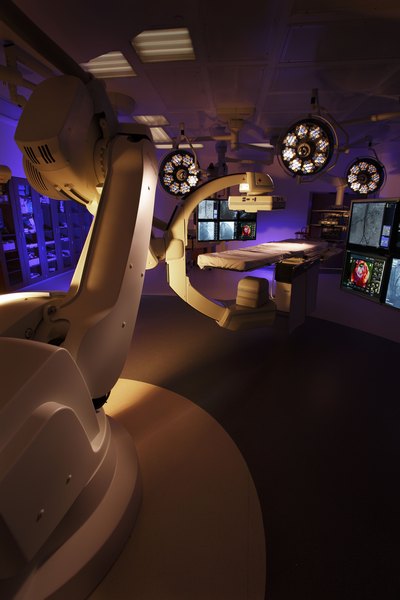
As an example, one of the hybrid ORs at Nashville, Tenn.’s Saint Thomas Hospital is a 1,130-square-foot cardiac procedure room that supports the cutting-edge transcatheter aortic valve replacement cardiac procedure with the Edwards Lifesciences valve. The TAVR procedure allows patients not candidates for traditional open heart surgery to receive the life-saving heart valve replacement. Because of the precision required of the valve placement, the procedure can only be performed in a hybrid OR setting.
Studies have predicted that nearly 75 percent of cardiovascular surgeons will be working in a hybrid operating suite in the next three to five years. In fact, there’s an estimated 100 hybrid ORs already operational in the United States, according to the ECRI Institute. But designing a new hybrid OR for a hospital or medical facility is a complex task; one that involves plenty of advanced planning, strategic discussions and careful preparations.
Before an architect can put pen to paper and begin design drafts, there must be plenty of planning conversations with hospital leadership. First, the team must identify the suite’s intended function — the type of procedures it will support. The suite’s function guides all further planning, preparation and design. The next step is to identify the type of space needed to accommodate the suite and all its equipment and to determine its location within the medical facility. Is there an existing OR that could be renovated? Or will the suite require new construction? From there, the team identifies the staff that will use the suite and the medical equipment it will house. The designers also assess structural requirements, square-footage estimates and other factors, so each unique need is addressed before moving into the design and construction phases.
But the work doesn’t end there; because of the complexities of each hybrid OR and the technologies tied to the imaging component, the team tasked with construction needs to be constantly coordinating with the equipment vendor, facility and architectural/engineering team. This last push in effort makes the room achieve the initial planning goals.
The following timeline provides a rough idea of the duration of the different phases of creating a hybrid OR suite:
- 2 – 4 weeks: identify room function
- 4 – 6 weeks: equipment selection, site visits and vendor presentations
- 3 – 4 weeks: preliminary planning and site testing
- 4 – 6 weeks: schematic design (and preliminary vendor layouts)
- 4 – 6 weeks: design development
- 4 – 6 weeks: construction documents
- 4 – 6 weeks: authority’s review, contractor selection and permitting
- 4 – 8 months: construction
- 3 – 4 weeks: equipment commissioning and trials
A new hybrid OR could be up and running in about a year to a year-and-a-half. Suite sizes commonly range from 1,000-square-feet to 3,500-square-feet, with procedural rooms ranging from 650-square-feet to more than 1,100-square-feet.
Each facility will pose unique constraints and will support unique functions and procedures, but all hybrid ORs are the same. These spaces aim to improve patient safety and satisfaction by supporting the concerted use of cutting-edge surgical and imaging equipment in one centralized location. In helping medical facilities to streamline operations and improve care, they mark the next generation of advanced operating rooms and the popularity will likely continue to rise for many years to come.
David Magner, AIA, NCARB, EDAC, LEED AP, is a project architect in Gresham, Smith and Partners’ Nashville Design Studio. Magner can be reached at david_magner@greshamsmith.com. Angela Holcomb, AIA, NCARB, is a project architect in Gresham, Smith and Partners’ Tampa office. Holcomb can be reached at angela_holcomb@greshamsmith.com. To date, GS&P has designed 11 hybrid operating rooms nationwide, with seven others in progress.
Image of hybrid operating room at Saint Thomas Hospital in Nashville, Tenn. courtesy of David Bailey Photography.
Tags:
Posted July 17, 2012
More Articles:
- Coverings 2024
Apr 22, 2024 – Apr 25, 2024 - Hospital, Outpatient Facilities & Medical Office Buildings Summit
Apr 25, 2024 – Apr 25, 2024 - CxA Workshop & Exam
Apr 29, 2024 – Apr 30, 2024 - EMP Seminar & Exam at CxEnergy 2024
Apr 29, 2024 – Apr 30, 2024 - CxEnergy
Apr 29, 2024 – May 2, 2024 - PHCC West 2024
Apr 29, 2024 – May 2, 2024 - Lean in Design Forum 2024
May 1, 2024 – May 2, 2024










