Subscribe Now
Patient Safety and the Designed Environment
By Lou Bunker-Hellmich, Ph.D. and Terri Zborowsky, Ph.D.
The Institute of Medicine’s influential report, To Err is Human: Building a Safer Healthcare System, focused much-needed attention on patient safety. Recent research in healthcare design suggests changes to the physical environment may affect patient safety outcomes. While much work is still needed to build the body of knowledge on how patient safety and the designed environment intersect, here is what current studies suggest.
Patient Falls
According to the Institute for Healthcare Improvement, patient falls are among the most frequent and serious adverse patient safety events reported in hospitals. Falls frequently occur when patients get in and out of bed or use the toilet without assistance.
Specific design interventions that may reduce patient falls include:
• Minimal distances from the patient bed to the toilet;
• Handrails along the route to the toilet for patient support;
• Appropriate bed and toilet heights. Heights too high or those that are too low affect safe transfer and can increase patient falls;
• Decentralized charting to increase patient surveillance. Locate staff charting areas with views into patient rooms to increase visibility and access to patients;
• Generous family zones within patient rooms to facilitate frequent visits and overnight stays. Increased family presence can decrease patient falls and medical errors.
• Limited use of bedrails as they are ineffective in reducing falls and, may, in fact, cause more severe injuries than unrestrained falls.;
• Flooring selections that cushion falls. Carpet and rubber underlayment materials can reduce the severity of injuries suffered as a result of falling but can also increase tripping risk;
• Good lighting and reduced clutter in patient room.
Reducing Hospital-Acquired Infections
The Centers for Disease Control estimates that HAIs occur in 5 percent of all acute-care hospitalizations — affecting 1 out of 20 patients in the United States. Understanding the role of the designed environment in spreading infection (i.e., airborne and contact transmission) is an important step in reducing HAIs.
There is evidence indicating that HAIs may be reduced by:
• Providing single-bed patient rooms, which effectively prevent the spread of infection between patients;
• Conveniently located, highly visible hand-washing sinks and hand-gel dispensers to encourage good hand hygiene among staff;
• Improved air filtration (e.g., HEPA filters) and ventilation systems to prevent the airborne spread of infection;
• Specifying highly cleanable surfaces in patient rooms.
Patient-Room Layout
Another area where links between patient safety and the designed environment have been suggested is the layout of patient rooms. Two types of rooms — acuity-adaptable and standardized — are being utilized to address patient safety issues.
• Acuity-adaptable. Patient transfers and hand-offs are frequently associated with medical errors. Acuity-adaptable rooms are equipped to deliver varying levels of care to a patient in the same room, minimizing transfers and thereby improving safety. Unresolved issues with acuity-adaptable rooms include staff training and staff-to-beds ratios.
• Standardized. The concept of standardization in patient rooms draws on research originating in the aviation industry. Equipment and supplies are located in the same place in each patient room. According to proponents of this approach, because staff always knows where equipment and supplies are in every room, they are able to focus mental energy on care and may be less likely to make errors, especially in life-threatening situations (e.g., emergency department or intensive care). Research evidence to support this assertion, in the hospital setting, is not yet available.
Evidence-Based Design research has the potential to contribute to efforts to reduce the number of adverse events occurring in hospitals. Growing the body of research on patient safety and the designed environment is achievable with the collaboration of healthcare facility owners, managers and designers as they undertake well-conceived and thorough studies and share the results of research.
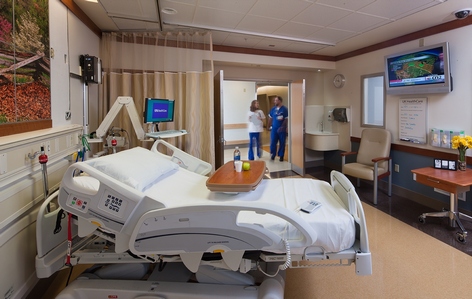
Photo Credit: Scott Pease/Pease Photography 2011
Lou Bunker-Hellmich, Ph.D., is a healthcare research specialist at AECOM. Bunker-Hellmich can be reached atlou.bunkerhellmich@aecom.com. Terri Zborowsky, Ph.D. is director of healthcare education and research at AECOM. Zborowsky can be reached at terri.zborowsky@aecom.com.
Editor’s Note: Stay tuned for the July/August issue of MCD, which features a Spotlight on safety and security.
Tags:
Posted May 17, 2011
More Articles:
- Coverings 2024
Apr 22, 2024 – Apr 25, 2024 - Hospital, Outpatient Facilities & Medical Office Buildings Summit
Apr 25, 2024 – Apr 25, 2024 - CxA Workshop & Exam
Apr 29, 2024 – Apr 30, 2024 - EMP Seminar & Exam at CxEnergy 2024
Apr 29, 2024 – Apr 30, 2024 - CxEnergy
Apr 29, 2024 – May 2, 2024 - PHCC West 2024
Apr 29, 2024 – May 2, 2024 - Lean in Design Forum 2024
May 1, 2024 – May 2, 2024










